in their first year of practice
College of Health and Behavior
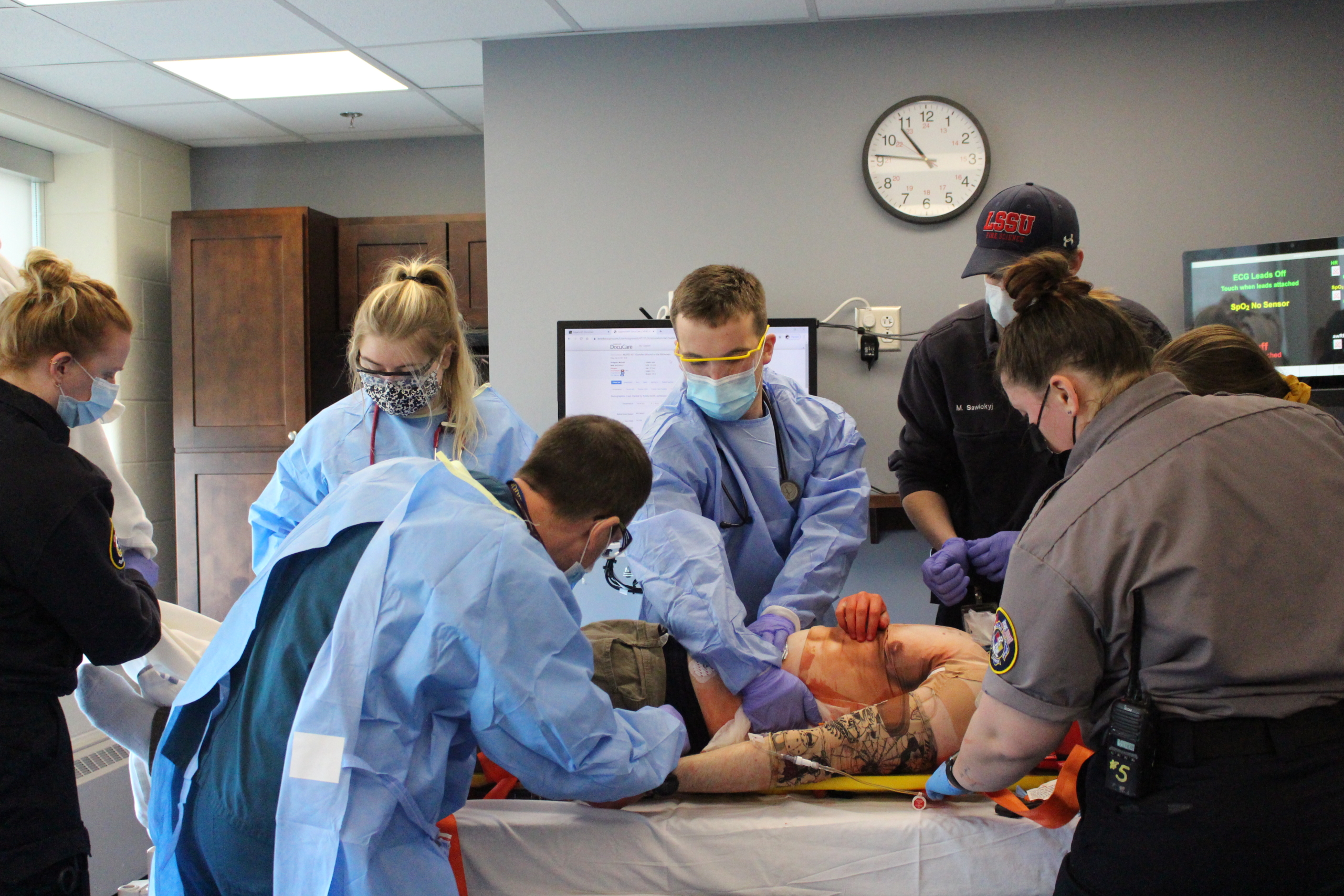
Rural Nurse
Residency Certificate Program
in their first year of practice
LSSU’s Post-Baccalaureate Rural Nurse Residency Certificate Program will graduate registered nurses equipped to address issues in retention, equity, access, and diversity in rural healthcare settings.
Nurses are in high demand, especially in rural settings, for various reasons. Many regions worldwide are experiencing a significant need for new nurses to fill vacancies, replace retirees, and address growing shortages. In particular, numerous rural hospitals face the risk of closure, with a substantial percentage of them at an imminent threat.
Lake Superior State University has taken steps to address this urgent need through its innovative educational approach to improving the presence of BSN prepared nurses in Rural settings. LSSU believes it is an important aspect of our social responsibility to do or part to address equity, access, and diversity in nursing and rural health settings. LSSUs Post-Baccalaureate Rural Nurse Residency Certificate Program, is one of a kind globally.
This competency-based program is designed to benefit BSN-prepared nurse residents in support of their transition to rural nursing practice throughout their first year post undergraduate graduation. This program offers advanced learning in critical thinking, conflict management, legal nursing, quality management, ethics, and leadership. Graduates of accredited BSN programs within their first year of practice, can earn this valuable credential in one year through cutting-edge academic instruction and paid full-time employment.
To cater to the needs of working nurse residents, LSSU has developed learning strategies that incorporate a mix of virtual, simulation, asynchronous, and synchronous experiences, along with hands-on healthcare experiences. Nurse residents are also paired with both a nurse mentor and a nurse preceptor to facilitate evidence-based learning and professional growth.
LSSU’s Post-Baccalaureate Rural Nurse Residency Certificate Program benefits newly graduated BSN nurses, rural communities, and the healthcare industry as a whole. By focusing on building confidence, competence, critical thinking, and clinical judgment (the four C’s), the program equips first-year nurses with additional skills to advance their careers. Simultaneously, it contributes to improving healthcare access in rural communities, helping alleviate some of the widespread inadequacies and improving access to care. Moreover, by increasing retention rates among BSN-prepared RNs in rural health care settings and reducing turnover, the program addresses nursing shortages prevalent in the healthcare sector.

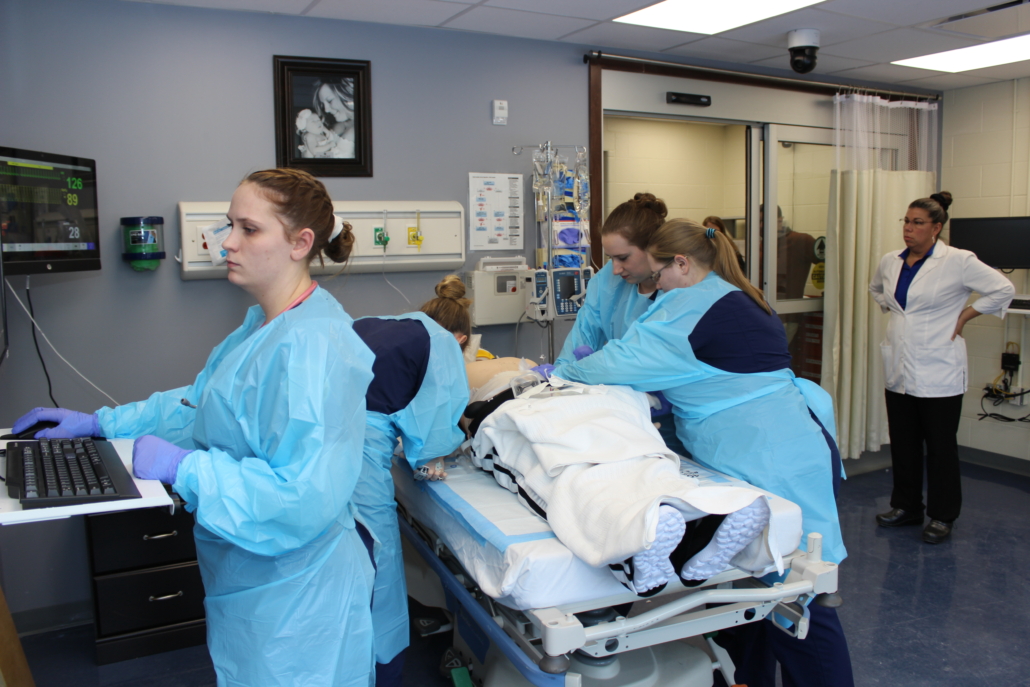
- 12-month program
- 24 credits virtual/hybrid
- 36 hours weekly employment
- Fluid entry points three times per year: May, September, and January
Rural Nurse Residency I (RNRP 501; 8 credit hours): Nurse residents explore and utilize skills learned in undergraduate nursing education to examine their role and responsibility in the practice environment. Through the use of simulation and actively engaging assignments, such as nursing grand rounds, residents begin to strengthen their confidence and competence in practice.
Rural Nurse Residency II (RNRP 502; 8 credit hours): Nurse residents broaden and regionalize their ability to apply evidence-based learning to practice. Critical thinking applications become more challenging as resident nurses become more experienced. Professional goals are established and a vision and outline for a professional framework in practice are developed.
Rural Nurse Residencey III (RNRP 503; 8 credit hours): Nurse residents universalize and affirm their transition to practice. Program mentoring and learning culminate in professional service engagement and completion of leadership experiences. Disparities and risk mitigation in rural health are identified through a final capstone project demonstrating improvements for access, equity, and diversity.
Outcomes for Nurse Residents who enroll in LSSU’s Post-Baccalaureate Rural Nurse Residency Certificate Program:
- Nurse Residents will develop a high level of independence and competence in rural health care settings
- Nurse Residents will develop increased confidence in both independent and collaborative rural nursing practice
- Nurse Residents will enhance their critical thinking and professional judgment abilities
- Nurse Residents will gain rural nurse leadership skills applicable to rural nursing practice
- Nurse Residents will develop their nursing role in relation to rural health policy
- Nurse Residents will demonstrate altruism, human dignity, and social justice by improving accessibility, diversity, and equity of healthcare in rural communities
Accessibility Statement
Lake Superior State University is committed to making reasonable accommodations related to its facilities, programs, or services for qualifying students, staff, faculty, and campus guests with disabilities as required by applicable laws. If any programming or activity is scheduled in an inaccessible space, requests for relocation shall be made to the Human Resources office at 906-635-2213, if possible, 48 hrs prior to the event. View Accessibility Statement Details







